Kenya Day 7: Waiting Rooms to Recovery Wards


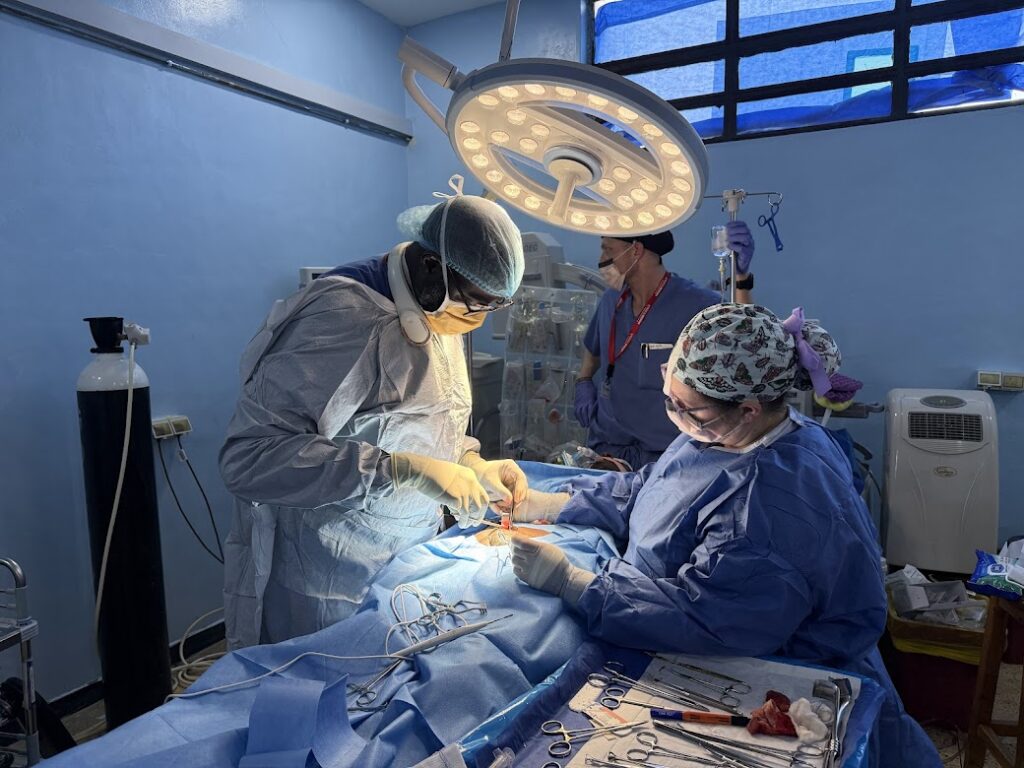
Thursday began in the quiet that follows an exceptionally long night. On Wednesday, the operating rooms ran continuously—case after case—until well past midnight. Our team did not leave the OR until 12:30 a.m. Thursday morning. By the time the hospital settled, recovery was already underway, and by morning, patients, families, and staff were returning to waiting areas and wards with the subdued focus that comes after sustained intensity. Thursday unfolded less around schedules and procedures and more around the people who had passed through them.
Jackline N., 40, lives with her husband Job and their five children on a small family farm about 20 kilometers from Nyamira. The land has been passed down through generations, and Jackline works it daily—tending maize, potatoes, tea, and coffee—while Job takes painting or construction work when it becomes available. Their home also includes two cows, a dog with puppies, and a rabbit. When asked what Jackline enjoys, Job said simply that she loves to work, go to church, and help others.
About a year ago, Jackline began to tire more easily. Over time, Job noticed she breathed heavily while sleeping, woke drenched in sweat, and was constantly thirsty. Walking long distances became difficult, and eventually swelling appeared in her neck. When they heard about our surgical outreach on the radio, they came for screening on Sunday, hopeful that answers—and help—might finally be within reach.
Dr. Stan Augustin diagnosed Jackline with a goiter and scheduled her for surgery on Wednesday. The procedure itself went smoothly, and half of the goiter was removed without complication. In recovery, however, Jackline’s condition changed quickly. She began shaking and appeared confused. Her heart rate climbed rapidly. She was experiencing a thyroid storm, a rare and life-threatening surge of thyroid hormones that can send the body into metabolic crisis.
Dr. Emil Markulis, our anesthesiologist, intervened immediately. He administered medication and stayed with Jackline late into the night. Even after the rest of the team left the hospital just after midnight, he remained. The ICU was full, and Jackline needed close monitoring. Dr. Markulis stayed until space became available and the hospital team could safely assume her care.
By late Thursday morning, Jackline was awake and improving, though still disoriented, sitting alone in the ICU. She had not yet seen her sister Norah or her husband. Outside the unit, Norah and Job waited. They had spent the night there, and as hours passed without updates, fear took hold. They began to believe Jackline had died and that no one was telling them. When one of our team members approached, they asked only to see her body. No one had realized they had been denied access to the ICU.
Once the misunderstanding became clear, the team moved quickly and brought them inside. Jackline was sitting up in bed. Norah and Job reached her together—tears, laughter, hands clasped tightly. They stayed with her for a long while, feeding her snacks, reminding her to drink, sitting close. Relief settled quietly into the room.
___________

Just a few steps away, Deborah, age nine, waited in the pre-operative area with her father. She had been evaluated earlier in the week for an umbilical hernia and hyperdontia, a condition in which an extra tooth grows between the two upper front teeth. Her father shared that these issues had affected Deborah’s confidence for as long as he could remember. She often asked why she couldn’t look like other children. They had always hoped to address the problem, but opportunity had never aligned until now. Deborah is the middle child, with an older sister and a younger brother, and she loves to dance. When asked about it, she shifted her feet and wiggled her hips, moving to a rhythm she seemed to carry with her as she waited for care with Dr. Carol Ann Aylward.
____________





Another patient, “Sunshine,” 48, arrived at the hospital profoundly ill. She is HIV positive and had been bleeding continuously, leaving her weak, dizzy, and exhausted. Her blood count was 7 g/dL, dangerously low. Dr. Traci Johnson evaluated her and found multiple large fibroids, measuring roughly 8–10 centimeters. Sunshine needed a hysterectomy, but Dr. Johnson explained that surgery would not be safe without blood transfusion.

The following day, while rounding on another patient, Dr. Johnson found Sunshine seated nearby. Sunshine told her she was ready for surgery. When asked how that could be possible, Sunshine explained that she had returned to her community and asked for help. Three people volunteered to donate blood. Each gave one unit, which she received overnight. Her lab results confirmed it—she was now stable enough to proceed.
As the team prepared, Chrissy Whitworth, our nurse and scrub technician, noticed abnormalities in Sunshine’s cervix. Further examination revealed a low-lying fibroid involving the cervix. Without the proper equipment and follow-up care, proceeding would have carried a serious risk of catastrophic bleeding. The surgery was stopped. Dr. Johnson explained the decision carefully and clearly. It was not safe to continue—not here, not now.

Chrissy and daughter, Vivian
The disappointment was immediate. Sunshine had done everything asked of her. Her community had come through. Relief had felt close. But this was not a refusal—it was a pause. Sunshine still needs surgery, and when the team returns with the proper equipment and support, that care can be provided.
Thursday unfolded in moments like these—relief alongside restraint, progress alongside pause. Care did not always mean completion. Sometimes it meant staying late, explaining difficult decisions, sitting quietly with families, and committing to return with what was still needed.

Pass my regards to Dr Emil Marculis. He stayed till 3am while I was looking for a bed in ICU while he was taking care of the patient with thyroid storm. He looked at me and said , Edna , lay at the coach as I monitor the patient. Rest a bit. It was really thrilling working with the whole team.